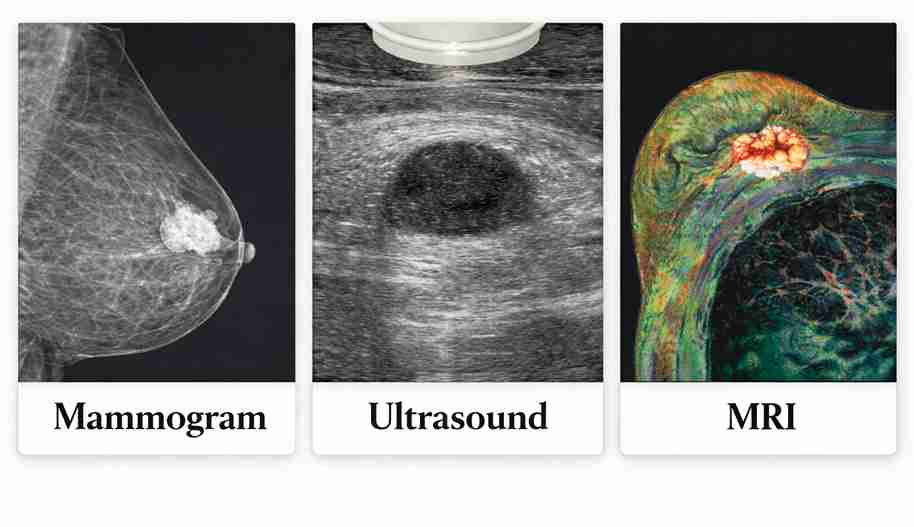
Mammograms are the standard screening tool, ultrasounds assess lumps and dense breast tissue, and MRI is reserved for high-risk or unclear cases, providing detailed imaging when other tests do not give definitive answers.
Breast cancer detection isn’t a one-test game. Mammograms, ultrasounds, and MRIs each serve a specific role based on age, breast density, symptoms, and individual risk. Choosing the right test improves accuracy and reduces unnecessary procedures.
For those seeking breast cancer screening, consulting an experienced breast cancer doctor ensures the right imaging approach, leading to earlier detection, clearer diagnosis, and more confident treatment decisions.
Which test is usually used first (and why)
A mammogram is typically the first screening test, whereas symptoms often require a mammogram followed by an ultrasound. MRI is added only in selected situations.
Screening (no symptoms): mammogram is usually first-line
It is the backbone of every breast cancer screening test in Kolkata and across India. For women without symptoms, mammography remains the global standard screening tool. It detects early calcium changes that are undetectable by physical examination.
Key reasons mammograms come first:
- Proven to reduce breast cancer deaths
- Detects very early changes
- Fast and widely available
- Uses low radiation
Symptoms (lump/pain/discharge): ultrasound + diagnostic mammogram are common starting points
When a patient presents with a lump, pain or discharge, doctors combine imaging. Truth be told, this mammogram vs ultrasound for breast lump decision is not either-or. Both are used together to understand structure and texture.
High-risk or unclear cases: MRI is often used to add detail (not replace everything)
MRI is not a replacement test. It is a problem-solving tool. It adds clarity in high-risk patients, unclear mammograms, or treatment planning.
This is where the discussion of mammogram vs MRI breast screening becomes relevant, because the decision depends on clinical risk rather than technology preference.
Are you screening or checking a symptom?
Screening is meant for women without symptoms. Any lump, pain, or discharge requires targeted diagnostic imaging rather than routine screening tests.
If you have a new lump, here’s what most doctors order first
- Diagnostic mammogram
- Targeted breast ultrasound
- Biopsy only if imaging suggests concern
If you’re asymptomatic: what “screening” means (and what it doesn’t)
Screening means testing for breast cancer before symptoms appear to catch disease early and improve outcomes. It does not diagnose cancer by itself or replace evaluation. Any abnormal finding still needs targeted tests and clinical correlation.
Women seeing a breast cancer doctor for routine screening often discover that early detection leads to simpler treatment and better survival.
Red flags: when you should not “wait and watch”
Certain signs require immediate evaluation. Waiting can delay safe treatment.
So ACT FAST when you notice
- Bloody nipple discharge
- Skin dimpling
- Rapid swelling
- Hard fixed lump
- Fever with redness
What to do next (appointment + imaging plan)
Next steps include booking a consultation with a breast cancer doctor, reviewing your risk profile, and creating a personalised imaging plan. This may include -Mammogram, ultrasound, or MRI based on symptoms, age, and breast density.
Mammogram: what it detects best
Mammograms are designed to catch very early calcium changes long before a lump can be felt. This makes them the most effective tool for early breast cancer detection and routine screening.
How mammography works (X-ray) and what it’s great at: microcalcifications
Mammography uses low-dose X-rays to detect microcalcifications. These may be the first signs of cancer. Most digital mammography centres now provide high-resolution imaging.
Screening vs diagnostic mammogram: what’s different
- Screening: routine check
- Diagnostic: focused exam with extra views
Limitations: dense breasts can reduce sensitivity (but mammograms still matter)
Dense breast tissue can mask cancers on mammograms, reducing sensitivity. However, mammograms remain essential, and a dense breasts ultrasound after a mammogram is often recommended to improve detection when visibility is limited.
Breast ultrasound: when it’s the right tool
Breast ultrasound is ideal for evaluating lumps, confirming cysts, and guiding needle tests. It adds clarity when mammogram findings need targeted, real-time imaging support.
Best use: distinguishing cyst vs solid lump and guiding needle tests
Ultrasound helps doctors quickly tell whether a lump is fluid-filled or solid. This clarity guides safe needle testing and prevents unnecessary procedures.
It helps doctors:
- Confirm harmless cysts
- Evaluate solid masses
- Guide biopsies safely
Dense breasts: ultrasound as a supplement (not a replacement for mammogram)
Ultrasound supports mammography in dense breasts. It adds information but does not replace screening.
Limitations: why ultrasound alone can miss certain early signs
Ultrasound cannot reliably detect microcalcifications. Therefore, it is not a replacement for screening.
Breast MRI: when it’s worth the extra detail
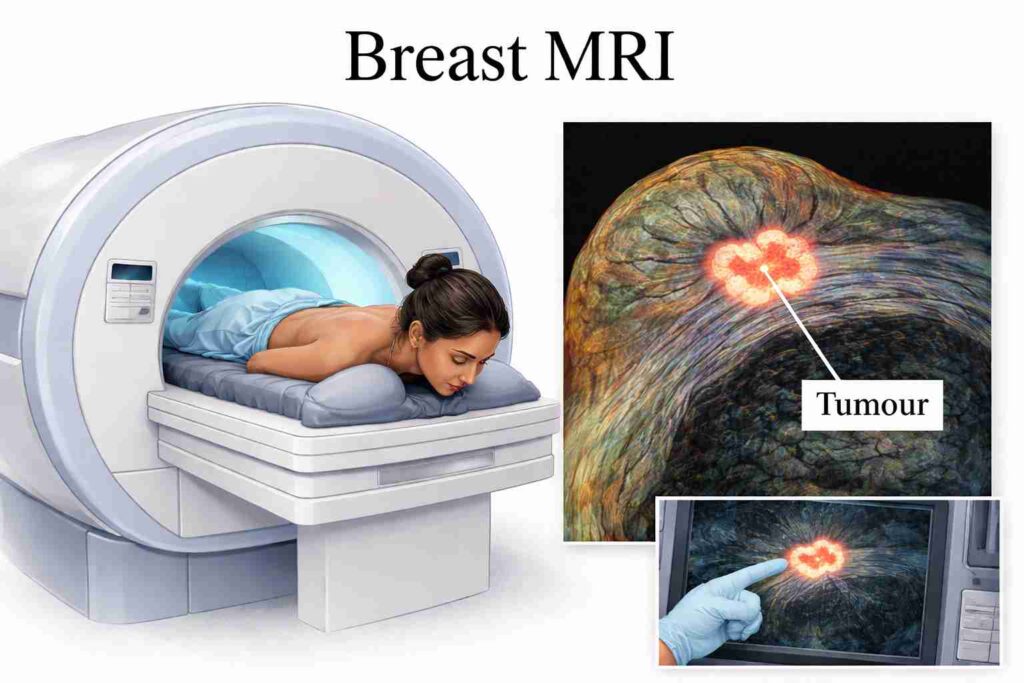
Breast MRI is reserved for high-risk screening and complex cases. It provides more detailed imaging when standard tests cannot fully explain suspicious or unclear findings.
Best use: high-risk screening, problem-solving, extent mapping, and implant evaluation
MRI is valuable for:
- Genetic high-risk patients
- Unclear mammograms
- Mapping tumour spread
- Implant checks
The question of breast MRI screening for high-risk individuals and who needs it inevitably becomes important. It helps doctors identify which patients truly benefit from advanced imaging.
Dense breasts + supplemental imaging (where MRI fits when available)
Dense breast tissue can hide important details on standard imaging. In high-risk patients, MRI provides greater clarity and may reveal findings that mammography or ultrasound may miss.
Limitations: false positives, contrast use, cost/time
MRI may:
- Detect harmless findings
- Require contrast injection
- Cost more
- Take longer
MRI is powerful but selective.
Mammogram vs Ultrasound vs MRI: comparison table (fast decision aid)
Each test serves a different clinical role. The table below explains the differences between Mammogram, Ultrasound, and MRI:
Best for / misses / typical use case / time / comfort / radiation / contrast
| Feature | Mammogram | Ultrasound | MRI |
| Best for | Early calcium changes, routine screening | Checking lumps, cyst vs solid | High-risk detail, complex cases |
| Misses | Can be limited in dense breasts | Early calcium changes | Can show false alarms |
| Typical use case | Screening + diagnostic follow-up | Lump evaluation, biopsy guidance | High-risk screening, problem-solving |
| Time | 10 minutes | 15 minutes | 30–40 minutes |
| Comfort | Brief compression | Generally comfortable | Longer, enclosed scan |
| Radiation | Yes, very low dose | No | No |
| Contrast | Not needed | Not needed | Usually required |
Common real-world combos
- Mammogram + ultrasound for symptoms
- Mammogram + MRI for high-risk screening
Which test do you need?
Many patients ask which test is best for breast cancer detection. Doctors choose imaging based on age, symptoms, breast density, pregnancy status, and personal risk. This structured pathway ensures accurate detection while avoiding unnecessary tests or delays.
Age + symptom + pregnancy/lactation
- Under 30 with lump: ultrasound first
- Over 40: mammogram + ultrasound
- Pregnancy: ultrasound preferred
Breast density
Women with dense breast tissue may need supplemental ultrasound or MRI because dense tissue can hide abnormalities, making additional imaging important for safer, more accurate detection.
Family history / genetic risk / prior breast cancer
Patients with strong family history, genetic risk, or prior breast cancer often benefit from MRI screening alongside mammograms to improve early detection and treatment planning.
Breast implants
MRI is often used to assess implant integrity. Dr Suvadip Chakrabarti, a breast cancer doctor in Kolkata, personalises this decision.
What results mean: BI-RADS, callbacks, and when a biopsy is recommended
BI-RADS scores standardise breast imaging results, guiding next steps. Callbacks mean additional imaging is needed, not confirmed cancer. A biopsy is recommended when findings appear suspicious or unclear, to confirm whether cells are benign or malignant.
Why “called back” doesn’t automatically mean cancer
A callback usually indicates the image needs further review. Most recalls are precautionary, and most of these findings are found to be harmless after further testing.
How imaging leads to the next steps
Possible follow-up:
- Targeted ultrasound
- Extra mammogram views
- Needle biopsy
Speaking with Dr Suvadip Chakrabarti, a noted breast cancer specialist in Kolkata, explains the results clearly and avoids unnecessary fear.
How to prepare for each test
Preparation is simple and improves comfort.
Mammogram prep
- Avoid deodorant on test day
- Schedule after periods
- Take mild pain relief if needed
Ultrasound prep
- Wear a two-piece outfit for easy access
- Avoid applying lotions or powders on the chest
- And carry prior reports
MRI prep
- Metal screening required
- Contrast consent needed
- Claustrophobia options available
Where do Kolkata people get these tests, and what to ask the concerned specialist
Patients should choose an expert that combine modern imaging technology with clinical guidance. The goal is not just getting a scan, but getting the right interpretation and a clear next plan from an expert.
Questions that matter
Ask whether
- Digital mammography is available
- If a trained breast radiologist reads the scan
- How fast reports are delivered
- And whether biopsy support exists onsite
In case of an emergency, note that Dr Suvadip Chakrabarti provides mammography and breast MRI in Kolkata.
What affects pricing
- Equipment type
- Contrast MRI use
- Specialist interpretation
Consulting Dr Suvadip Chakrabarti, a breast cancer specialist in Kolkata, should guide the coordination of imaging through trusted facilities.
People Also Ask
Is an ultrasound enough if I have dense breasts?
No. Ultrasound complements mammography but cannot replace it, as mammography detects early calcium changes that ultrasound may miss.
Why would a doctor order an MRI after a normal mammogram?
MRI provides greater detail in high-risk patients or when findings are unclear and can reveal areas not visible on standard imaging.
Which test is best for a breast lump?
A combined mammogram and ultrasound provides the most accurate evaluation.
Does mammography cause cancer because of radiation?
No. Mammography uses extremely low radiation and has been shown to be safe.
Final Verdict
Mammogram, ultrasound, and MRI are not competing tests. They are coordinated tools. The best detection strategy uses the right sequence based on symptoms, age, and risk. Early imaging saves lives when guided by an experienced specialist.Treatment planning benefits from multidisciplinary care led by Dr Suvadip Chakrabarti, a breast cancer doctor in Kolkata, ensuring that imaging informs precise action.


